Aligning Care Delivery to Emerging Payment Models
Boards can employ a “maturity framework” to help their organizations evolve
By AHA Center for Health Innovation
Editor’s note: Excerpted from “Evolving Care Models,” a Market Insights report from the AHA Center for Health Innovation that provides an overview of the successes and challenges providers have experienced in aligning care delivery models with alternative payment models, and that provides lessons for those in the midst of this transition. As payers shift financial risk to providers through more advanced payment models, trustees will need to help their organizations build new capabilities for succeeding under these payment arrangements.
Hospitals and health systems across the country are redesigning care delivery to improve quality and outcomes, enhance the patient experience, reduce costs and, ultimately, produce better population health. They are testing and implementing new care models to focus on prevention and better coordinate care across the many sites of care that touch patients.
The payment landscape for health care services has evolved to support providers’ transition to new care delivery models. Over the past 10 years, payers have transitioned a growing portion of payments made to providers from traditional fee-for-service to alternative payment models (APMs). Also, commonly referred to as value-based payment models, APMs incent providers for quality and value, rather than volume.
The AHA Center for Health Innovation based this report on information and insights from a number of sources, including interviews with hospital and health system leaders and other health care experts, surveys of hospitals and health systems, and a number of health care reports and research articles.
Evolution in Care Delivery Models
Among other key points, the report’s collaborators have observed that:
- APMs vary in the degree of financial risk they transfer to providers, but most providers today still assume relatively low levels of risk. This approach provides stability to providers as they build up the required capabilities for taking on higher levels of risk.
- APMs have gained traction in recent years, driven in large part by government payers. Activity across commercial payers varies geographically but is also accelerating. In certain cases, public and private payers are working together — at both the national and state levels — to align payment models.
- Providers are juggling the challenge of developing the capacity to operate successfully in shared-risk payment models, while still caring for significant numbers of patients in fee-for-service arrangements.
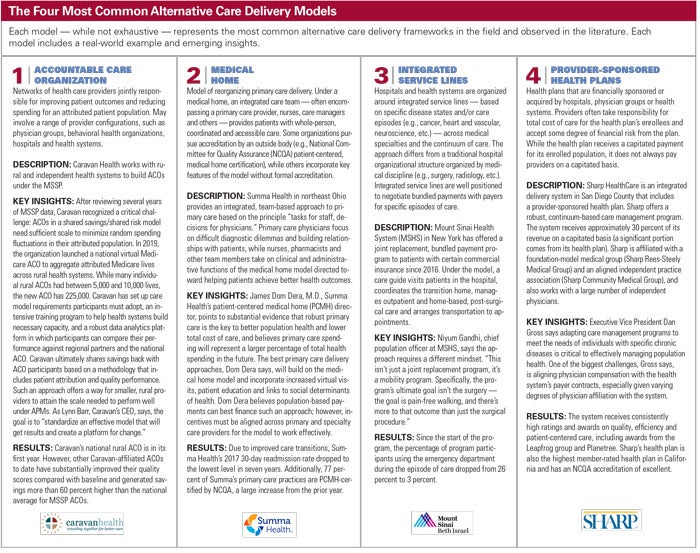
Four Most Common Alternative Care Delivery Models
Various service-delivery and payment models that aim to achieve better care for patients, smarter spending and healthier communities are still evolving and being tested. Health systems are implementing and refining a wide array of care delivery models. Alternative approaches have clustered around four specific models: accountable care organizations (ACOs), medical homes, integrated service lines (bundled payment programs) and provider-sponsored health plans.
According to the report, health systems without previous experience in alternative care delivery models chose to adopt one of the most common care models for the first time, and those with experience were adopting new processes and/or technologies to make the models more effective.
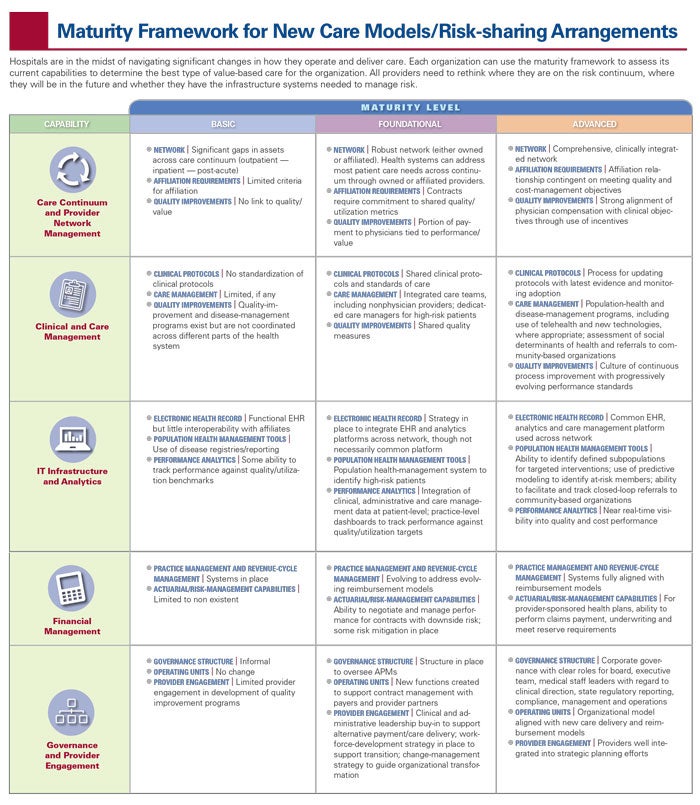
Maturity Framework for APMs
While government payers have sparked a paradigm shift during the past decade around how to pay for health care, they have allowed for a transition, granting providers time to build new capabilities without significant exposure to downside risk. Many health systems now find themselves with one foot in more traditional fee-for-service payment systems and the other in alternative-reimbursement models. They want to transform their care models, but struggle to finance the required changes to their networks, processes and support systems.
Boards can help their organizations evolve toward value-based payment models by employing a “maturity framework” in discussions with their leadership team, see pages 5-6.
Each organization can use the maturity framework to assess its current capabilities to determine the best type of value-based care for the organization. All providers need to rethink where they are on the risk continuum, where they will be in the future and whether they have the infrastructure systems needed to manage risk.
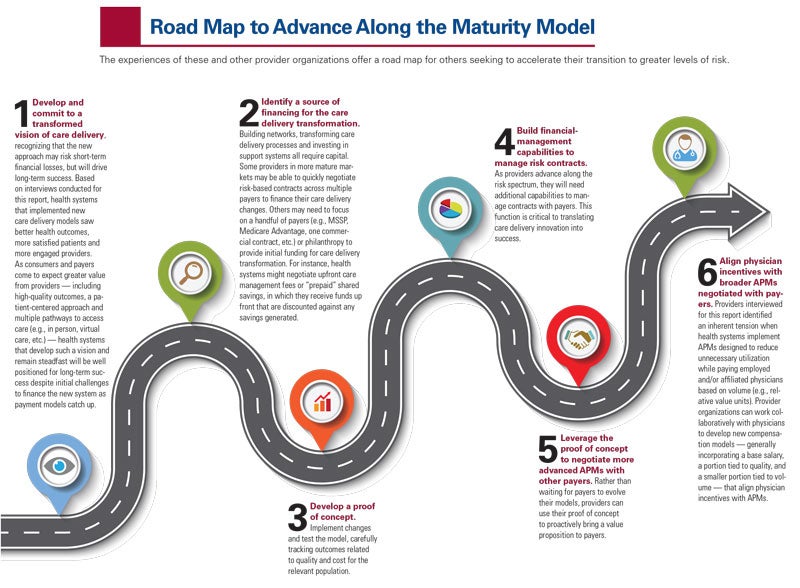
Road Map to Advance Along the Maturity Model
Health system leaders who have embarked on care delivery change say they are committed to continuing the evolution toward value-based care because the approach is better for patients, but they caution that there is no silver bullet that can substitute for: setting an inspiring vision for care delivery; engaging clinicians to agree on evidence-based protocols and care plans; retraining staff to support the new approach; and building feedback loops to measure organizational performance and adjust accordingly.
The following “road map” offers leadership lessons for those wishing to transform their care models.
Conclusion
By building care delivery prototypes, testing their models and bringing a value proposition to payers, health systems can achieve greater alignment among reimbursement from government and commercial payers, thereby further accelerating care delivery transformation. Such an approach creates a virtuous cycle where initial successes in care delivery and payment reform provide feedback to drive bolder care model changes and increased levels of financial risk. As payers continue to shift higher levels of risk onto providers, hospitals and health systems that can leverage this positive feedback loop to transition a substantial portion of their payment stream to APMs will be well positioned for success. Through the hard work of changing their care models, providers are poised to lead care delivery change to improve patient outcomes.