Executive Performance and Compensation
Key Action Steps for the Compensation Committee
Take time in 2019 to reexamine your executive compensation program
By Timothy Cotter and Kathryn Hastings
Practical
Governance
Trustee Talking Points
- Anticipated retirements and increasing competition for executives with the skills necessary to lead transformation may create talent shortages.
- The compensation committee should review the executive compensation program to ensure its relevance for the changing environment.
- Pay equity within the organization’s executive group is emerging as an important focus area for the committee’s deliberations and training.
- Shared performance goals at the system level are becoming more common in order to support alignment and encourage collaboration.
As health care organizations face a number of emerging challenges, the compensation committee of the not-for-profit hospital or health system board is well served to review and update the executive compensation program periodically. Key action steps on which to focus for 2019 include:
Assess the executive compensation program in the context of a rapidly changing environment.
Health care is changing rapidly. In response, hospitals and health systems are evolving the scale and scope of their operations. New executive roles are emerging, and system roles are growing in organizationwide impact, while selected roles, often at the subsidiary hospital level, are narrowing in scope. Consequently, health care leaders should consider whether their current executive compensation programs are still the best fit. Questions to consider include:
- Is the executive compensation philosophy appropriate for the changing environment?
- Is more flexibility required to support attraction and retention?
- Does the organization’s peer group reflect its actual competitors for executive talent?
- Is the mix of fixed versus variable cash compensation appropriate?
- Are retention devices required for select executives?
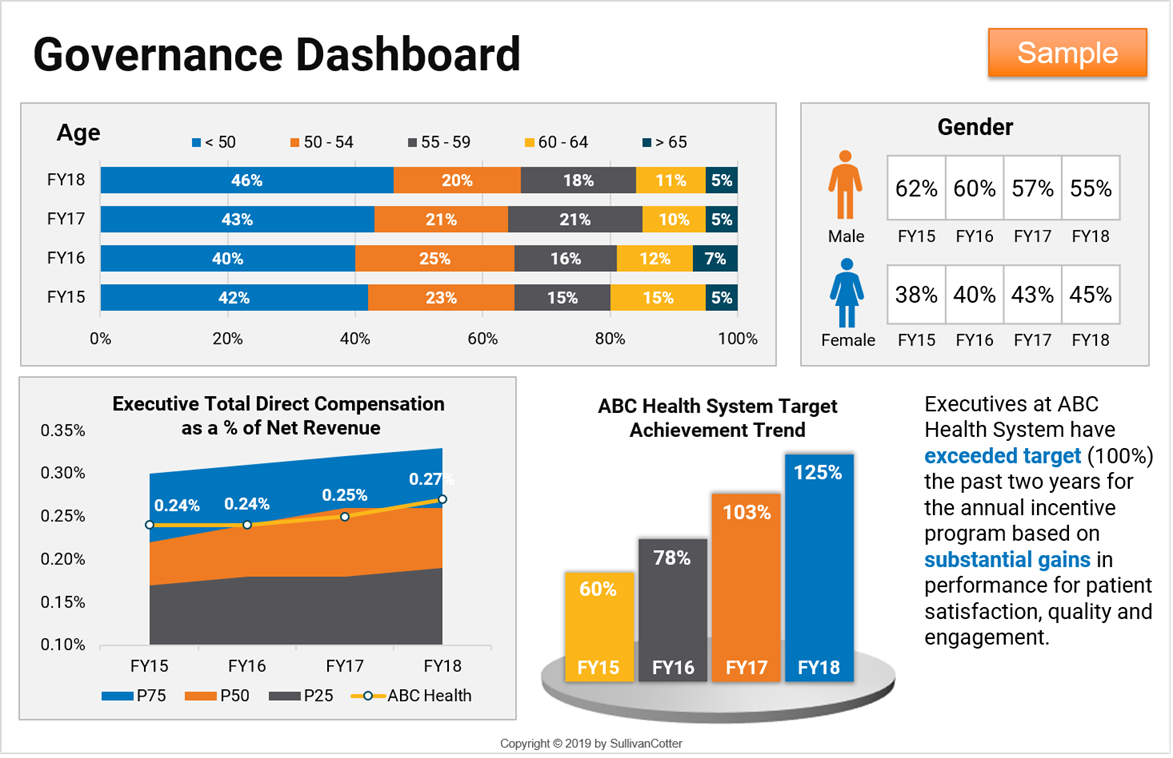
Develop a governance dashboard to ensure the program is not drifting in unexpected directions.
To support oversight, the board compensation committee should develop a dashboard that focuses on executive compensation-related outcomes measured over multiple years. By tracking outcomes, the committee can ensure that the program operates consistently with the established philosophy and that areas requiring attention are readily identified. When combined with comprehensive tally sheets and affirmation that all executive compensation arrangements are fully disclosed to the committee, there is a comprehensive baseline underlying the committee’s deliberations. Such longitudinal measures focus on program metrics, demographics, performance outcomes and recruitment/retention. Examples include:
- Structure and demographics, such as the number of executive positions, age and tenure distribution of the executive team, and diversity in executive roles.
- Actual market position versus the target for base salary, total cash compensation, total direct compensation and total compensation.
- Executive compensation expenditures as a percentage of hospital/health system expenses or net operating revenue.
- Average executive salary increases, with and without market adjustments, versus those of non-executives.
- Incentive award payouts (annual and longer term) as a percentage of target.
- Number of executives recruited from or leaving for peer group, health care and general industry organizations.
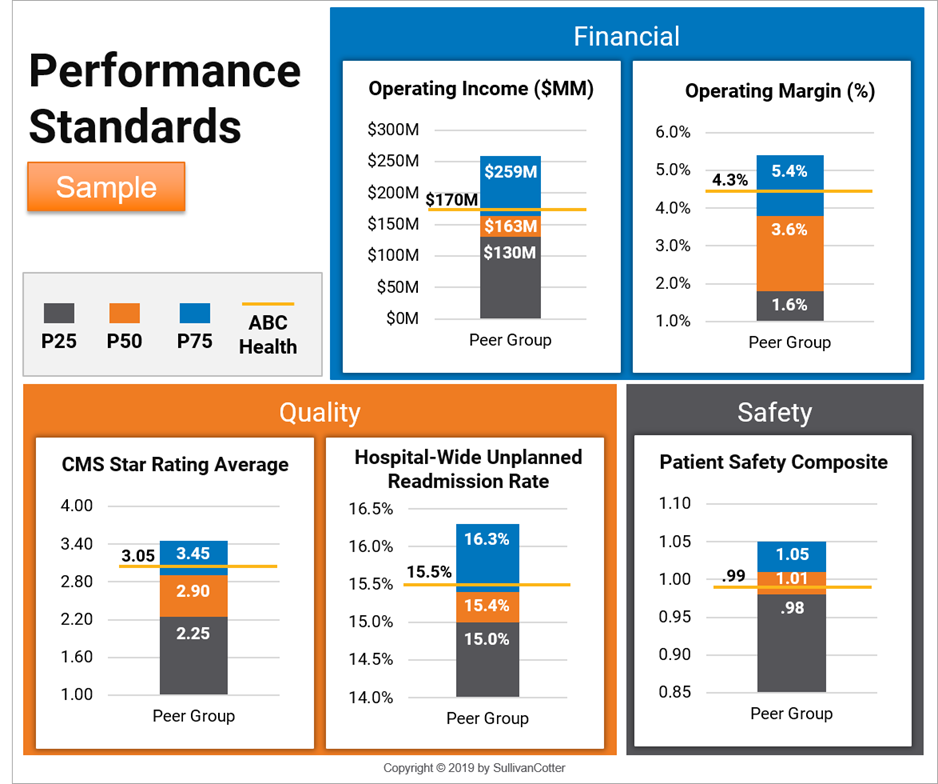
Evaluate the annual incentive plan to ensure an optimal measurement focus.
According to SullivanCotter’s 2018 Manager and Executive Compensation in Hospitals and Health Systems Survey Report, annual incentive plans (AIPs) are the norm (84 percent prevalence). With evolving organizational strategies and greater transparency regarding performance, the board compensation committee should review and, if appropriate, enhance AIP performance measures. Questions to review include:
- Do the measures align with the organization’s key objectives in a value-based environment? The survey indicates the most commonly used AIP measures include:
- Quality
- Patient engagement
- Patient safety
- Financial results
The survey also reports increasing use of the following AIP measures:
- Efficiency
- Access
- Lives under risk contracts
- Condition-specific process outcomes and measures
- Is the focus of performance measurement at the appropriate level? The SullivanCotter survey indicates an increasing focus on shared goals at the system level rather than at the subsidiary hospital level in order to support alignment and encourage collaboration.
- How much “stretch” is included in the performance standards? The committee should ensure that some or all of the same organizations that compose the compensation benchmarking peer group are considered when establishing performance standards for the incentive measures. Relative performance data abstracted from audited financial statements, Centers for Medicare & Medicaid Services Star Ratings and value-based programs and the like can help to ensure the resulting executive compensation levels are aligned with organizational performance and that AIP metrics are set considering the actual performance levels of peer institutions.
Determine the feasibility of a long-term incentive plan.
As hospitals and health systems expend greater resources to help achieve long-term goals, a focus beyond annual performance is required. Long-term incentive plans (LTIPs) are typically limited to the organization’s most senior executives. The performance periods of LTIPs are typically three years and focus on strategic objectives that support alignment and important long-term goals such as growth, integration and financial stability. The longer performance periods also support executive retention and team stability, especially if the for-profit sector is a key talent market.
According to the SullivanCotter survey, 30 percent of not-for-profit health systems with revenues greater than $1 billion use LTIPs. For systems with revenue greater than $5 billion, prevalence approaches 60 percent.
Link executive compensation to strategic talent management.
Anticipated retirements and increasing competition for executives with the skills necessary to lead transformation may create talent shortages.
To support strategic talent management, the board compensation committee, working with the chief executive officer (CEO), the chief human resources officer (CHRO) and the board committee with talent management responsibilities should consider processes that:
- Assess the competitiveness of the current compensation arrangements of potential internal candidates for the organization’s most senior roles, as these individuals are likely to be the subject of recruitment efforts.
- Periodically evaluate the compensation of candidates given their ongoing development and fit versus the desired senior executive profile.
- Ensure the compensation provided to the successful internal leadership candidate reflects market competitive levels.
- Include measures in the AIP that address the CEO’s, CHRO’s and candidates’ effective participation in the talent management process.
Review compensation arrangements for executives outside of their core organizational responsibilities.
The board compensation committee, working with the board committee that addresses conflicts and the chief compliance officer or the general counsel, or both, should review the compensation paid to executives for roles outside of their core organizational responsibilities as well as the related responsibilities and time commitments, given the potential for significant adverse stakeholder reaction to real or perceived conflicts. This review should include:
- Compensation related to the executive’s efforts when representing the not-for-profit organization’s interests in ventures with for-profit organizations, which should be assessed for reasonableness and conflicts of interest and commitment.
- Outside employment income for roles not related to the not-for-profit hospital or health system, which should be evaluated to ensure executives are fully focused on their primary roles and that potential conflicts are identified and addressed.
Examine pay equity in a broad context.
Pay equity is emerging as an important focus area for the board compensation committee. There is no universal best practices strategy; therefore, the committee should consider the following activities as they relate to the executive population:
- Work with the CHRO and the general counsel to gain a preliminary understanding of the state of pay equity within the executive group.
- Use more advanced techniques, rather than a comparison of means/medians and distributions of base salary and total cash compensation across employee groups, to identify potential pay inequities. Such factors as education level, external experience, internal experience, job performance and related variables can provide a better understanding of pay inequities and better support remediation activities.
- Consider additional actions that will support pay equity long term, such as the use of consistent starting salary standards, salary bands that group jobs by contribution and impact, an assessment of how leave-of-absence policies impact compensation, and leadership talent strategies for underrepresented populations.
- Ensure training, tools and guidelines that promote pay equity are provided to compensation decision makers.
Trustee Takeaways
- Discuss whether any new, expanding or narrowing executive roles are well served by the current compensation program.
- Adopt forward-looking techniques for tracking compensation-related outcomes and determining potential pay inequities.
- Consider program updates, e.g., a long-term incentive plan for certain leaders, to support executive retention and team stability.
- Identify potential disclosure issues likely to draw media and stakeholder attention, and be prepared to respond accordingly.
Identify the potential for external scrutiny of committee decisions.
External scrutiny of executive compensation is to be expected as the cost of health care continues to grow and compensation levels increase.
The board’s compensation committee should be mindful of:
- Total compensation that is at the top end of amounts reported on the Form 990 by stakeholder-perceived peers.
- Significant severance payments, especially when contemporaneous media reports indicate the executive’s departure was voluntary or for cause.
- Significant increases in compensation for executives when the organization is perceived to be struggling financially and the workforce has been negatively impacted (e.g., layoffs, pay freezes).
- Large lump-sum payments of deferred compensation earned over multiple years.
- A compensation approval process that does not obtain the rebuttable presumption of reasonableness.
- Perquisites that do not support the executive’s job responsibilities directly.
As part of its decision-making process, the committee should identify the potential disclosure issues its decisions may create. Committees will find it helpful to review pro-forma Form 990s to understand the disclosure implications of compensation arrangements under consideration, identify forthcoming disclosures likely to draw media and stakeholder attention, and ensure required media and public relations preparations are completed.
Support the hospital or health system mission.
As organizations realign their strategic objectives with a rapidly changing health care environment, executive compensation programs are evolving in kind. To help ensure these programs continue to support the organization’s mission, the board compensation committee should determine if corresponding actions or updates are necessary.